
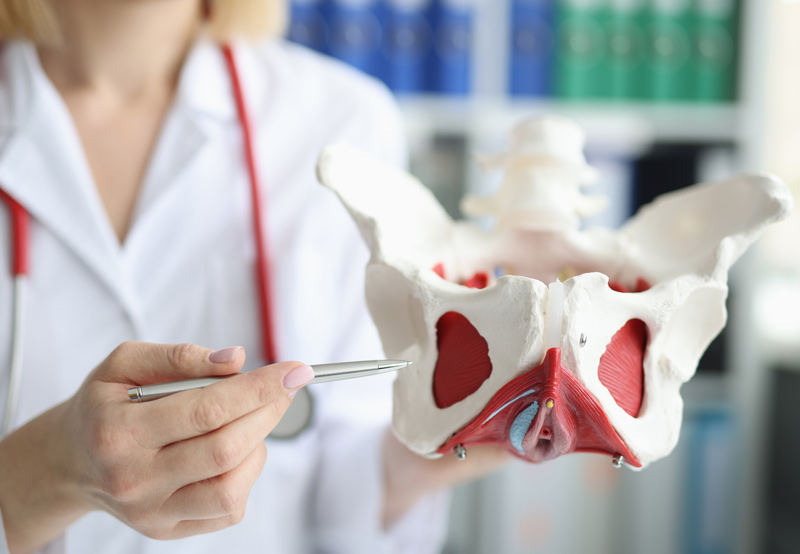
Pelvic organ prolapse (POP) refers to a condition in which the normal support of the pelvic floor has weakened and the anterior vaginal wall, posterior vaginal wall, and or the apex of the vagina have descended.
Symptoms of Pelvic Organ Prolapse
Women may experience back pain, pelvic pressure, splinting, pelvic pain, and the sensation of a bulge. In addition, patients may struggle to pass stool, feel unable to completely empty the bladder, and experience fecal urgency or incontinence.
The most common symptom of POP is a bulge outside the hymen.

Risk Factors of Pelvic Organ Prolapse
The following factors may increase a woman’s risk of developing pelvic organ prolapse:
- Infant size
- Vaginal parity
- Advanced maternal age
- Caucasian or Hispanic ethnicity
- Operative delivery (forceps, vacuum)
- Estrogen status
- Pelvic surgery
- Increased abdominal straining (caused by obesity, smoking, and lung disease)
Treatment for Pelvic Organ Prolapse
It’s important that treatment for POP doesn’t cause more harm than benefit. Women who aren’t experiencing bothersome symptoms of POP or the presence of a bulge should undergo routine exams. The exceptions are women who develop urinary retention that leads to overflow incontinence or recurrent UTIs.
Women experiencing pelvic pressure, heaviness, or the sensation of something falling out of the vagina will benefit from physical therapy. Myofascial release will help strengthen the core, which includes the hips, back, and abdomen, improving symptoms of pelvic pressure and urinary incontinence.
Pessary treatment can be used in short-term situations until a woman can undergo surgery. A pessary is a silicone intravaginal device designed to provide support to the descended organs. Most women are able to remove, clean, and place pessaries themselves. Pessaries should be removed and left out overnight two to three times a week.
Obliterative surgical procedures are for women who no longer desire sexual intercourse due to medical comorbidities, advanced age, or lack of a partner who has functional erections. Reconstructive surgeries, however, don’t impact vaginal length.
If the patient chooses reconstructive surgery, then the surgeon will explain the benefits and complications of abdominal versus vaginal surgery, the use of synthetic meshes, and mesh complications.
Colpocleisis is an obliterative, transvaginal procedure for women who do not want to preserve the option of vaginal intercourse. A total colpocleisis involves the removal of the vaginal epithelium, whereas a partial colpocleisis involves a partial removal to provide drainage tracts in a woman with a uterus. Some patients may need to undergo Pap smear testing and endometrial evaluation prior to surgery.
Sacrospinous ligament suspension (SSLS) is a reconstructive vaginal surgery performed on women with apical prolapse. During surgery, the physician will use permanent or delayed absorbable sutures to make a transvaginal suspension of the vaginal apex to the sacrospinous ligament. The complications of this procedure include gluteal pain, anterior vaginal wall prolapse recurrence, and post-operative dyspareunia.
Vaginal uterosacral ligament suspension (USLS) involves attaching the vaginal apex to the bilateral uterosacral ligaments using permanent sutures. Complications of USLS include nerve injury, suture erosion, and ureteral obstruction.
Transvaginal mesh procedures may also be done to treat pelvic organ prolapse.

